Introduction
- Types:
- Mechanical Valves
- Ball-in-cage
- Single tilting Disc
- Bi-leaflet
- Advantages:
- Very durable (ideal for young patients)
- Disadvantages:
- Higher thrombotic risk
- No transcatheter options (all surgical)
- Bioprosthetic Valves
- Made of pericardial/bovine/cadaver tissue
- Advantages:
- Low risk of thrombosis, many not require anticoagulation
- Some can be inserted minimally invasive (i.e. Transcatheter – TAVR)
- Disadvantages:
- Earlier wear/degeneration (generally ~ 10y longevity)
- Internists MUST appreciate types of mechanical valves to understand anticoagulation targets
- Internists may not need to know difference in types of bioprosthetic valves.
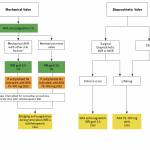
- Mechanical Valves
Mechanical Valve Types
| Ball-in-Cage | Single Tilting Disk | Bi-leaflet Tilting Disk | New Generation Bi-leaflet Tilting Disk |
|---|---|---|---|
 |  | 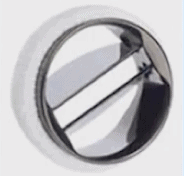 |  |
| Starr-Edwards | Bjork-Shiley | Medtronic bileaflet | On-X Valve |
|
|
|
|
Bioprosthetic Valves
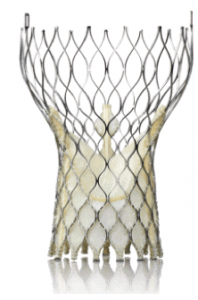
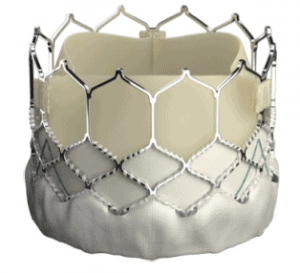
| Surgical Valves | Transcatheter Self-Expanding (TAVR) | Transcatheter Balloon Expandable (TAVR) |
|---|---|---|
 |  |  |
|
|
|
Complications of prosthetic valves
- Paravalvular leak (regurgitation around the valve)
- Valve stenosis (i.e. pannus ingrowth)
- Patient prosthesis mismatch (i.e. valve is too small for patient’s size, leading to functional stenosis)
- Valve thrombosis (can present with stroke)
- Valve endocarditis
Anticoagulation / Thrombotic Risk
- All prosthetic valves have a risk of thrombosis.
Mechanical Valves
- Risk of thrombosis:
- Mechanical
- Mitral position (Tricuspid position – VERY high risk)
- Other thrombotic risk factors (AF, low LVEF, prior embolism)
- ALL patients with mechanical valves require LIFELONG anticoagulation with a vitamin K antagonist (Warfarin) (DOACs are contraindicated)
- ASA 81mg daily for MOST patients with mechanical or bioprosthetic valves (unless contraindications exist)
| INR Target | Cases |
|---|---|
3.0 | Most cases (esp mitral/tricuspid positions) |
| 2.5 | Need ALL Of: |
1.5-2.0 + ASA (≥ 3mo | Need ALL Of: |
** INR target is 0.5 above and below single digit above
Bioprosthetic Valves
- Surgical Bioprosthetic AVR
- Post-Op 3-6mo: VKA (warfarin) with INR target 2.5 for 3-6mo
- Lifelong: ASA 81mg daily
- Transcatheter (TAVR)
- Post-Op 3-6mo: ASA + clopidogrel OR VKA (warfarin with INR target 2.5)
- Lifelong: ASA 81mg daily
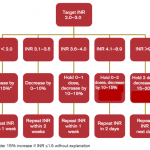
Trips for managing INR
- (See Thrombosis Canada for a detailed guide)
- Do not reverse supratherapeutic INR with vitamin K without clinically significant bleeding. (INR < 10)
- INR > 10 consider reversal in some clinical situations
- INR takes 3-7 days to respond to a dosing change, which is the time taken to metabolize clotting factors.
- Common drugs that increase INR:
- Antibiotics/antifungals (esp. quinolones)
- Amiodarone
- Statins (except atorvastatin/pravastatin)
- Acetaminophen > 1g/day
- Levothyroxine dose changes
- ASA and NSAID drugs combined with warfarin increase risk of bleeding, but generally do not affect INR
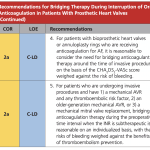
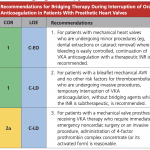
Bridging for surgery
- Bridging is not required for minor dental procedures (dental extractions, cataract procedures)
- Patients with bileaflet valves in an aortic position with no risk factors for thrombosis generally do not require bridging. Their anticoagulation can be interrupted for procedures, and re-intiated.
- NOTE: These are generally patients who have an INR target of 2.5 or 1.5-2.0.
- Patients with an INR target of 3.0 generally need bridging due to high risk of thrombosis. However, decisions must be individualized.
| Bridge (Individualize) |
|
| No Bridge |
|
Emergent Surgery
- For patients requiring emergent surgery, reversal with 4-factor prothrombin concentrate (PCC) is recommended and restarting anticoagulation as soon as possible after surgery
Further Reading
Authors
- Primary Author: Dr. Pavel Antiperovitch (MD, FRCPC Cardiologist)
- Secondary Author and Reviewer: Dr. Atul Jaidka (MD, FRCPC Internal Medicine)