General Overview
- An Infection of the inner layers of the heart most commonly involving the valves.
- Infection can lead to destruction of the valve resulting in a number of cardiac complications including valvular insufficiency, heart failure, heart block, death.
- In addition, valve destruction and infection can cause embolism’s which can cause complications such as stroke, renal/splenic infarcts,and peripheral bacterial seeding.
Risk Factors
- Preexisting valvular disease
- Congenital heart disease
- Prosthetic valve
- Intravenous drug use
- Hospitalization
- Previous infective endocarditis
- Central line
Microbiology
- Staphylococcus Aureus
- Streptococcus Viridans
- Coagulase-Negative Staphylococcus
- Streptococcus Bovis
- Enterococcus
- HACEK Organisms ( Haemophilus, Actinobacillus, Cardiobacterium, Eikenella, Kingella)
- Fungal (Candida species)
Diagnosis
| Definite Endocarditis | Possible Endocarditis |
|
|
| Major Criteria | Minor Criteria |
|
|
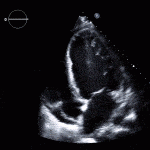
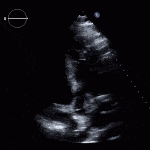
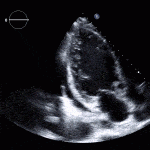
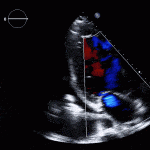
Role of Echocardiography
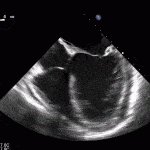
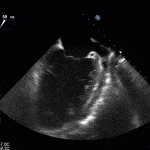
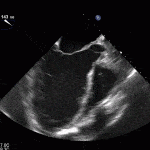
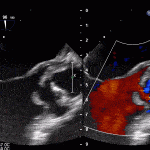
- Echo plays an important role in the diagnosis of infective endocarditis.
- Helps identify vegetations, new valvular lesions, abscess, and other complications of endocarditis.
- Class I:
- Transthoracic (TTE) should be performed in all cases of suspected infective endocarditis
- Class I:
- Transesophageal (TEE) should be performed if TTE images are inadequate or ongoing suspicion for infective endocarditis.
- If a high degree of suspicion for infective endocarditis despite a negative TEE, the TEE should be repeated in 3-5 days.
- If new cardiac complications develop after the initial TEE, the test should be repeated to look for new intracardiac complications.
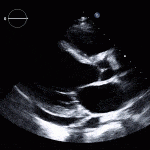
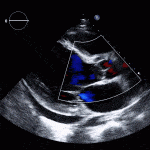
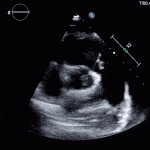
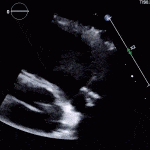
Case 1
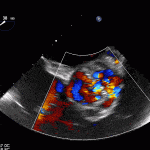
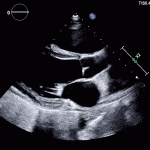
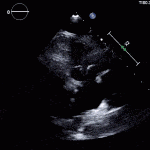
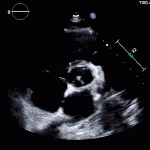
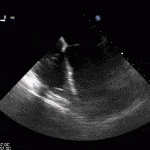
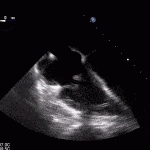
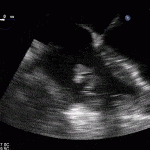
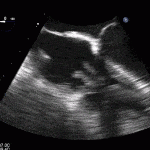
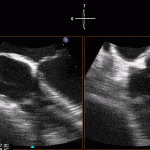
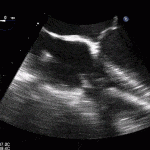
35 year old male with history of intravenous drug use presents to hospital with fever and shortness of breath. On Auscultation there is a loud diastolic murmur best heard at the LLSB on end expiration.
Transesophageal Images
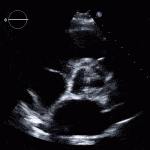
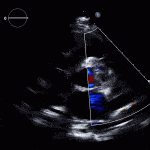
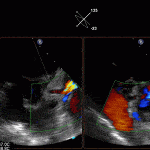
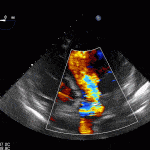
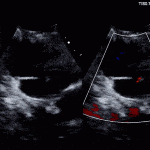
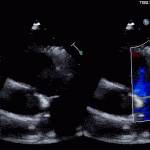
Case 2 (Pulmonic Valve IE)
Diagnosis of Cardiovascular Implantable Electronic Device (CIED) Infections:
Class I:
1. All patient with 2 positive blood cultures should be started on prompt antibiotics for CIED infection.
2. Generator pocket tissue as well as lead tip should be sent for gram stain and culture when explanted.
3. All Patients with suspected CIED should undergo TEE to asssess for infection on leads as well as vegetations on valves.
Class IIa:
1. Patients should seek assessment by cardiologist or infectious disease expert should they develop unexplained blood stream infection.
Class III:
1. Percutaneous aspiration of generator pocket should NOT be performed for diagnosis assessment.
Management of Cardiovascular Implantable Electronic Device Infections
Class I
1. Removal of device and lead is recommended for all patients with definite CIED infection. This includes pocket infection such as abscess, erosion of the device, skin adherence, chronic draining sinus.
2. Complete device and lead removal is recommended for all patients with valvular endocarditis without definite involvement of the lead.
3. Occult staphylococcal bacteremia removal of the device and lead is recommended.
Class IIa
1. Reasonable to remove the device and lead if persistent occult Gram-negative bacteremia despite antibiotic therapy.
Class III
1. Removal is not needed for indicated for a superficial or incisional infection.
2. Relapsing bloodstream infection due to a a non-CIED source for which long-term suppressive antimicrobials are required removal is not required.
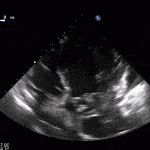
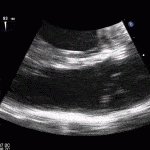
Case 3
Treatment
- Consult infectious disease specialist for optimal antibiotics therapy.
- Cardiac Surgery consult if complications from infective endocarditis and consider for prosthetic valve endocarditis.
- Generally 4-6 weeks of appropriate antibiotics.
Indications for Surgery
- Valve dysfunction causing congestive heart failure (Class I).
- Left-sided endocarditis with resistant organisms such as fungal or Staph Aureus (Class I).
- Endocarditis with evidence of abscess, heart block, or destructive lesions (Class I).
- Persistent infection of 5-7 days or more after initiation of appropriate antibiotics (Class I).
- Prosthetic valve endocarditis (PVE) with relapsed infection (Class IIa).
- Persistent vegetations and/or Recurrent emboli despite appropriate antibiotics: usually defined as enlarging vegetation, ongoing fever, or positive bacteremia 7-10 days despite antibiotics (Class IIa).
Timing for Surgery
- Patients should be operated on within days (Class I).
- Patient should be on appropriate antibiotics at time of surgery (Class I).
- Once on appropriate antibiotics further delay in surgery is unlikely to be beneficial (Class IIa).
- A delay of 3 weeks is reasonable in patients with recent intracranial hemorrhage (Class IIa).
Further Reading
- AHA/IDSA 2015: Infective Endocarditis in Adults: Diagnosis, Antimicrobial Therapy, and Management of Complications (html) (pdf)
- 2015 ESC Guidelines for the management of infective endocarditis: The Task Force for the Management of Infective Endocarditis of the European Society of Cardiology (ESC) Endorsed by: European Association for Cardio-Thoracic Surgery (EACTS), the European Association of Nuclear Medicine (EANM) (html) (pdf)
- Update on Cardiovascular Implantable Electronic Device Infections and Their Management: Larry M. Baddour Et al.Circulation. 2010;121:458–477